WE GET RESULTS THAT MATTER TO PATIENTS
2019 (Continued):
-
Medicare Changes Way It Pays Doctors, Helping Advance Integrated Care:
On November 1, 2019 the Centers for Medicare & Medicaid issued a Final Rule that includes changes to its physician payment policies, payment rates and quality measures for services provided by doctors and other practitioners under the Medicare Physician Fee Schedule effective 1/1/20. This FinalRule includes the following changes beneficial to primary care teams seeking to integrate behavioral health services into their practices:
— reduces the documentation burden on physicians and other care-team practitioners;
— broadens the practice role of practitioners who work with physicians as part of care team, e.g. RNs APRNs, PAs, etc;
— prioritizes treatment of opioid use disorders;
— adds new payment codes to list of allowed tele-health services, and
— increases payment for patient care coordination and care management.
Finalized Policy, Payment, and Quality Provisions Changes to the Medicare Physician Fee Schedule for Calendar Year 2020 -
Kaiser Permanente Launches PHQ-9s in Its Clinics.
The growing presence of PHQ-9 patient surveys in primary care clinics is an important development and first step on a continuum of change, adding mental health services to patients care in medical settings. On completing the 9-question survey, patients can identify behavioral, emotional, mental health issues to talk to their doctor about. It will be a universal survey so that all patients will be asked to complete it. There is no stigma to its use. We know talking about behavioral problems can be difficult for patients to raise, and for doctors to discuss, so the PHQ-9 gives a science-based impetus for this discussion to begin. The PHQ-9 is a sign it is OK, in fact encouraged, for patients to bring up their behavioral issues with their PCP, e.g. depression, anxiety, phobia, etc. So that physicians can then assess, develop a treatment plan and consult with behavioral specialists as needed to provide behavioral health care. We are redefining health to include behavioral health and the PHQ-9 is an exciting early sign of progress! PHQ – 9 Form
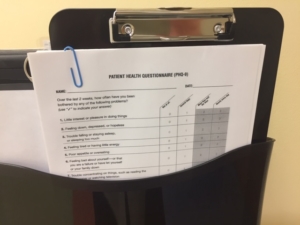

- July 2019 Medicare/Medicaid (CMS) announced that, starting in January 2020, it will begin paying medical practices for virtual psychotherapy, delivered via video-conferencing, as part of a bundled payment (i.e. per patient per month payment) to physicians for opioid use disorder treatment. CMS also proposes to begin paying medical doctors for substance use disorder services delivered via tele-health, again as part of a bundled payment. And where CMS leads, private commercial insurance companies usually follow in paying for such services.
- New Harris Poll shows majority of Americans now think mental disorders are nothing to be ashamed of and can be treated effectively.
- In a Harris poll commissioned by the American Psychological Association, it is clear the American public has moved significantly towards greater understand of mental disorders and acceptance of fact that effective treatments exist for behavioral conditions and should be accessed when needed. These changes in U.S. popular opinion reveal two things:
- The work of advocacy groups like NHMH and others are having a real effect, and as more Americans seek mental health care, NHMH’s mission becomes all the more critical: to ensure that effective, evidence-based care will in fact be available to them in primary care, when they seek that care.
https://www.apa.org/news/press/releases/2019/05/mental-health-survey
2018:
- Behavioral health services into primary care was one of the four Chronic Care policies that Medicare implemented through the calendar year 2017 physician fee schedule rule.
- Congress passed into law The Chronic Care Act of 2018 which includes provisions to pay primary care practices for integrated care services delivered to Medicare patients.
2017:
- Medicare agreed to pay medical practices for providing some elements of the integrated care model called collaborative care;
- NHMH persuaded the main federal agency, the Department of Health & Human Services, to hold the first-ever HHS-wide integrated care conference where all federal agencies doing integrated care (e.g. Veterans, Indian Health Services) reviewed findings and best practices;
2016:
- Federal Government’s Center for Medicare & Medicaid agreed to allow same-day billing for medical practices where patient received physical and behavioral health services in one visit;
-
Congress enacted The 21st Century Cures Act which requires the Asst. Sec. for Mental Health to submit a report every 2 years on inter- and intra-agency coordination efforts across all programs including bi-directional integrated care.
3 years ago
3 years ago
3 years ago
4 years ago
NHMH – No Health without Mental Health
www.nhmh.org
We work for a future where you can see a trained, qualified mental health professional for a consultation in the privacy of your primary care doctor’s office.4 years ago
It's Time to Mandate Treatment of the Dangerously Mentally Ill
www.commonsense.news
What happens when we leave people with psychosis to their demons? Ask the families of Alison Russo-Elling, Nathaniel Rivers, and Michelle Go.NHMH – No Health Without Mental Health a 501(c)3
Non Profit.
San Francisco – Washintong DC
RESOURCES
Publications
Glossary of Terms
Links
Sign Up for the NHMH newsletter
Stay up to date with the latest news & developments.
© 2019 NHMH. All rights reserved.
Privacy Policy



